Learning objectives:
- Understand some of the factors that contribute to the experience of shame in medical encounters.
- Be able to describe how shame, humiliation, and trauma are related.
- Identify the risk factors for developing traumatic stress reactions after medical encounters, specifically after ICU stays or pediatric hospitalization.
- Learn more about how shame and trauma affect both parties involved in the use of physical restraints.
Abstract:
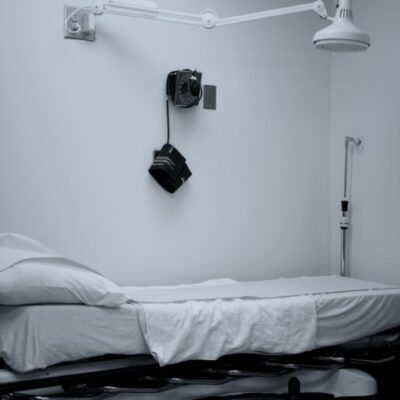
In this show, we explore the shame and trauma that patients can experience as a result of encounters with the medical or mental health systems. The potential for these emotional responses often goes unnoticed or unrecognized by professionals. This discussion was inspired by the work of Dr. Aaron Lazare, who devoted part of his career to raising awareness about the patient’s experience of shame and humiliation in medical encounters. We expand this topic to include several examples of medical-related trauma, with personal stories to highlight the lasting stress reactions that may result from these experiences. These conversations reveal the pervasive nature of shame and trauma, which occur even when working to help and heal others. We discuss the importance of recognizing the contributing factors for these reactions, in order to prevent or minimize their impact on patients and families.
Outline
- [1:00] Aaron Lazare on navigating shame between doctors and patients.
- [9:00] Dr. Nancy Kassam-Adams on the trauma of childhood medical procedures.
- [27:43] Nancy Andrews on experiencing PTSD after being in the Intensive Care Unit.
- [45:40] Bob Stains on the trauma of using restraints in psychiatric settings and how we talk to people who have hurt us.
Full Interviews Featured in this Episode
Shame Between Doctors and Patients
Aaron Lazare
Pediatric Medical Trauma
Nancy Kassam-Adams
PTSD in the Intensive Care Unit
Nancy Andrews
Restraints in Mental Hospitals
Bob Stains
Discussion Questions:
- In your own experiences as a patient, have you ever felt ashamed or humiliated? How do you think things could have gone differently to prevent those emotions?
- Imagine you have a child in the hospital or family member in the ICU, would you discuss ways to minimize trauma with the medical team?
- Dr. Lazare provides some examples of how the language we use can inadvertently lead to feelings of shame for patients. Can you think of other language we use or situations we put patients in that may lead to shame and/or humiliation?
- One potential method of reducing post-ICU PTSD is creating an ICU diary. This is a written account maintained by the medical team and patient’s family of the events that occured while the individual was in the ICU. How do you think this could help prevent post-ICU PTSD?
Links to additional resources:
Health Care Toolbox
Resource for providers to help children and families cope with illness
After the Injury
The Children’s Hospital of Philadelphia resource about pediatric medical trauma and supporting recovery
National Child Traumatic Stress Network
Organization raising the standard of care for traumatized children and their families
SAMHSA: Seclusion
Alternatives to seclusion and restraint from the Substance Abuse and Mental Health Services Administration
ICU Diaries Help Prevent PTSD (video)
Video from Johns Hopkins Medicine about the utility of ICU dairies in preventing post-ICU delirium
Articles:
“Shame and Humiliation in the Medical Encounter,” Aaron Lazare
“Nightmares After the ICU,” Jan Hoffman
From the New York Times Well Blog about the Johns Hopkins study examining PTSD post-ICU
“Rethinking Hospital Restraints,” Ravi Parikh
From the Atlantic